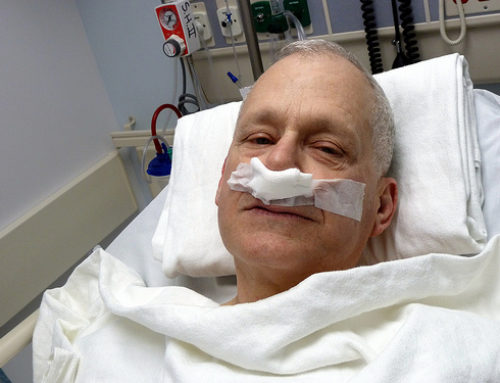
This list was compiled by a group of ARDS survivors and family members who thought about things that were done for them, or they wished would have been done for them, when they finally got out of the hospital.
Not everything will be right for you or your loved one; they are just suggestions of things that might make the transition from the hospital or rehabilitation facility back home, an easier journey. Congratulations for becoming another ARDS miracle.
Transition (Going Home)
- Ask the Occupational and Physical therapist what types of therapy devices might need to be in the home.
- Before you go home, measure the height of the toilet seat. Most are a standard 15 inches; some are 19 inches, and this difference will matter to a patient who is deconditioned.
- Check the bathroom to see if there are any support bars for the patient to hold on to when using the toilet.
- Make appointments with physicians prior to going home that you know you will need to make for follow up, such as with the pulmonologist, the ENT to check the trach incision, your internist, your thoracic surgeon. Try to set up out patient Physical Therapy and, if you get it, Occupational Therapy, so that you can begin as soon as possible.
- Try to have any prescriptions that the patient will need filled for the patient prior to or when they arrive home.
Patient concerns
- After spending such a lengthy time in the hospital, patient’s hair is dull, skin is dry. Help your loved one with a manicure, pedicure, general body pamper. Buy your loved one’s favorite shampoos, conditioners, body lotions, hand cream.
- Loose clothing that is easy to put on and take off.
- Shoes that would be comfortable for person who is newly homebound, be they gym shoes or flat, sturdy shoes to allow solid footing.
- A Night Light-adjusting to being home after being in the hospital for such a lengthy duration of time takes time, and sometimes people will be staying in rooms other than their bedrooms, due to stairs.
Information Exchange
- Every patient is different. Even if you think your loved one is one of those people who will want to know everything that has happened the second they come out of their coma, this might not be the case this time. Consider the fact that your loved on may be disoriented, confused, overwhelmed, and afraid. Too much information at one time is not always a good thing.
- Some patients have memory and/or comprehension problems, making it difficult to take in too much at a time. Remember this and have patience.
- Some patients have had very vivid dreams, feeling that they were so close to death and are not ready to “talk” about this experience, especially when they are still on a vent, and communication is so difficult.
- Some patients find the communication issue so frustrating, they find that the recovery process is going very slowly, and to discuss what has happened to them is too much for them right now.
- There will be some patients who, after recovering from ARDS, will never want to know too much about the syndrome, only the minimum. This sort of life threatening experience effects people in different ways, at different times in their lives. Some people will find, one or two years after coming home from the hospital, that this is the time they would like to learn more about the syndrome. If they need time to digest what has happened to them, give it to them. Everyone’s lives have changed as a result of the ARDS, but no one’s more than the survivor.
Friends & Family
- When your loved one is coming home, make sure that the first couple of days are subject to restricted visits and restricted numbers of visitors.
- Family and friends are understandably most eager to visit, but it can be very overwhelming and extremely taxing to deal with all the questions and hugs and kisses, although understood and greatly appreciated, the close proximity of many people can be exhausting at first. A bit of space and time is needed to readjust. Rest is badly needed at this time.
- Provide a map of the neighborhood (Yahoo maps or Mapquest.com) with names of friends and phone numbers and addresses. It would be helpful to notify the neighbors about the person coming home, especially if the patient lives alone.
- Coordinate efforts for people to cook and/or send food to the patient to minimize the amount of cooking that the patient has to, especially in those early days.
Personal Care
- A doughnut cushion can be beneficial. For patients who have been in bed for weeks or months, it makes it easier, more comfortable, for sitting, and getting up.
- Extra books and magazines. For some people who are finding it initially difficult to read, books on tape will be a nice change from the television.
- A good supply of soothing Cough lozenges, or Chloreseptic spray, (Vicks, Bradasol etc). Most patients who have been intubated or had a trach, come out of the hospital with their throat raw, with nasty coughs, or both.
Special Support devices
- A stool with wheels, to move from place to place around the house.
- A portable commode, to keep near the patient’s bed at night.
- Relaxation tapes to help patient relax and sleep; many ARDS survivors have a difficult time falling asleep or staying asleep.
- Acquire a raised toilet seat.
- Acquire a reacher. (Those things you use in OT to help you reach things and pick things up)
- Acquire a tape recorder and portable CD player.
- Get a book bag to carry stuff around. It helps if you walk with a cane for a long time. Also if you are hauling around oxygen.
- Get a big calendar for the kitchen so all information regarding medications, doctor and therapy appointments can be posted. Being extremely efficient with schedule keeping is most important. Keep in mind, some post ARDS patients may have memory problems and will need help with keeping their schedules; this may become an issue regarding medication, especially if someone lives alone.
- Find out which local stores have wheel chairs or Amigos and electric doors. This makes shopping easier for those who are not yet steady on their feet.
- Contact a support group in your area for pulmonary concerns. Contact the local American Lung Association who should have that information. There are groups called “Better Breathers” where you can meet other people who are on oxygen. There are pulmonary rehab programs where there will be others on oxygen. Though most areas do not have an ARDS organization, there will be other lung related groups that can offer support.
Going out
- A Cushion in a shopping bag. Some people lose so much weight that they find the seats in public places are so uncomfortable. Placing a cushion in a shopping bag was unobtrusive and helps to maintain some sense of normality and comfort until one can gain a sufficient amount of weight.
- Many post ARDS patients do not look sick, even though they are seriously deconditioned, fatigued, weak, and disabled. It is difficult for those, especially the post ARDS patients who are in their twenties, thirties, forties, even fifties, where the only real sign of their ARDS might be a tracheotomy scar. Some don’t even have the scar. But they are still feeling the effects of this serious syndrome and when they go out and have to face remarks from strangers who wonder why they are in a wheelchair, why they have a handicapped placard, it can be very frustrating. Especially when no one in the general public understands ARDS.
Home Maintenance
- Many people find being short of breath to be most distressing. Often, an inexpensive fan, with cool air blowing will helped people feel they are receiving more oxygen, but many find the psychological benefits to be tremendous.
- Some people find that having the furniture raised up on to wooden platforms was helpful so that they could get up out of them. The platforms were probably about eight inches tall, and placed underneath the bed, a couple of the chairs, and the couch.
- Replace the standard shower head with a handheld shower head. Since many people will be taking a shower sitting down, this will be easier.
- Install shower bench or chair. Some are adjustable and can be easily set up or moved. Or get a step stool that can be placed in the shower to sit on while showering.
- Move appliances that are used all the time down to the counter so they are easy to reach.
- Take advantage of online grocery shopping and home delivery during your recovery time, especially if you live alone or live with one person who has to go back to work relatively quickly. Many grocery stores and general merchandise stores have motorized shopping carts as well.
- Have phone jacks installed into different rooms in the house or invest in inexpensive cordless phones, at least one for each floor that you can keep with you at all times. They have them for about $19.99.
- Have cable TV put in room where recovering person will be spending most of time. Unfortunately, in the weeks and months immediately following hospitalization, many post ARDS survivors find reading for long periods of time too taxing; they can only be physically active for so long, although, with work, each day, they will hopefully be able to extend that time period. Therefore, having a variety of television choices will make the person feel as though they are not just wasting their time in front of the TV.
©2003 Copyright ARDS Foundation
Photo by Rochelle, just rochelle